Radiotherapy Services
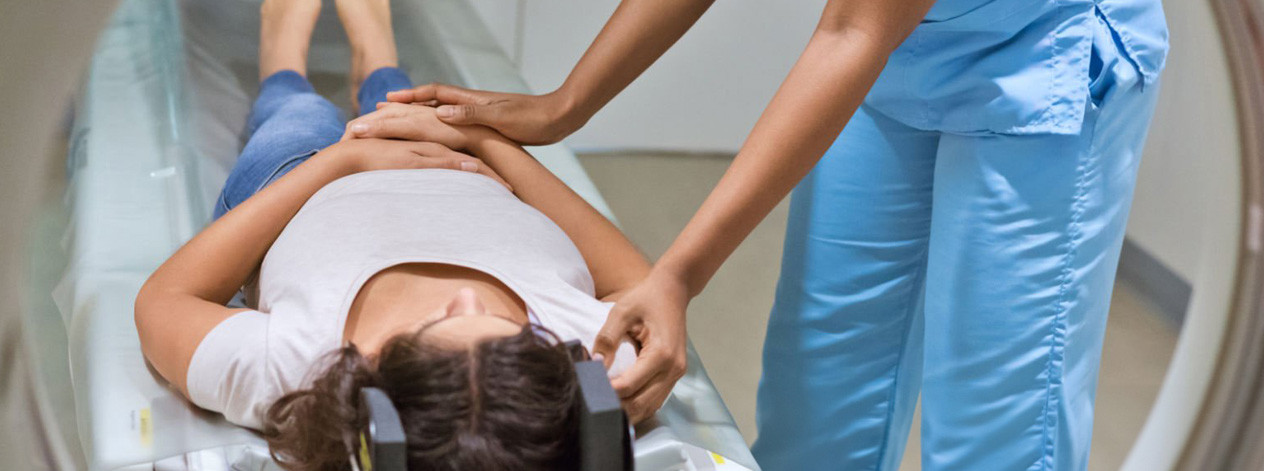
Radiotherapy uses targeted radiation to kill cancer cells. It can be used at different stages of treatment.
Oncology Consultants offers the most advanced standard of radiation therapy. Using localized high-energy rays, we can combat cancer cells and eradicate visible tumors, preventing them from growing and dividing, while minimizing side effects.
The radiation is delivered by a sophisticated machine called, Linear Accelerator. The machine has with image guidance technologies and stereotactic capability. We utilize advanced Cone Beam CT (CBCT) image guidance and Intensity Modulated Radiation Technology (IMRT) combined with non-invasive Stereotactic Ablative Radiation Therapy. Treatment Planning simulation for radiation therapy is performed using GE CT Discovery RT Gen 3 equipped with respiratory gating which enables 4-D planning for superior radiation treatment targeting.
WHAT TO EXPECT
Radiation therapy, also known as radiotherapy, is a common medical treatment used to treat various conditions, including cancer. It involves the use of high-energy x-rays that travel in a linear fashion to target and destroy cancer cells or shrink tumors. Here's what you can generally expect when undergoing radiation therapy:
Consultation and Planning: Before starting radiation therapy, you'll meet with a radiation oncologist who will review your medical history, conduct physical exams, and possibly order imaging tests such as CT scans or MRI to precisely locate the tumor. A treatment plan will be developed based on the type, size, and location of the tumor.
Simulation: During this step, you will undergo a simulation session where the treatment team will help you get into the exact position you'll be in during each radiation session. This helps ensure accurate targeting. The team will construct immobilization devices and place small marks (the size of a freckle) on your body to help algin your body in the same position for each treatment.
Treatment Schedule: Radiation therapy is usually given over a series of sessions, called fractions, which are spread out over several days or weeks. The number of sessions will depend on the type and stage of cancer, as well as the treatment goals. Most people receive radiation therapy as an outpatient procedure, meaning you can go home after each session.
Treatment Sessions: Each radiation therapy session is typically quick, usually lasting about 15 to 30 minutes. The actual radiation delivery takes only a few minutes, with most of the time spent ensuring precise positioning. You'll lie on a treatment table, and the machine delivering the radiation will be adjusted to target the tumor accurately. You will not be radioactive after treatment.
Side Effects: Radiation therapy affects both cancerous and healthy cells in the treatment area. Side effects can vary widely based on the location of treatment, the dose, and your individual sensitivity. Common side effects include fatigue, skin changes (redness, itching, or peeling), hair loss in the treatment area, and changes in the blood count. Your radiation oncology team will closely monitor your progress and manage side effects.
Managing Side Effects: Your radiation oncology care team will provide guidance on managing side effects. They might recommend creams or ointments for skin irritation, suggest dietary changes to combat nausea, or provide pain management strategies if necessary.
Follow-Up: After your course of radiation therapy is completed, you'll have follow-up appointments with your radiation oncologist to monitor your progress and assess the treatment's effectiveness. Additional tests or imaging may be ordered to evaluate the tumor's response to treatment.
It is important to have open communication with your radiation oncology team about any side effects or concerns you have during the treatment process. Everyone's experience with radiation therapy is unique, but the Oncology Consultants radiation oncology team is there to guide you and provide support throughout the treatment journey.
If you have any questions about radiotherapy, you can reach us at (713) 722-9660.
RADIOTHERAPY TYPES
A course of radiation where the dosage of each beam can be regulated, delivering high doses of radiation and minimizing the amount to healthy nearby tissue.
Radiation therapy technique that utilizes computer software and advanced machines to deliver radiation to precisely shaped targets in sites containing a tumor.
Tse Kuan Yu, MD, PhD:
Stereotactic Ablative Therapy (RT) is a modern way of delivering a high dose of radiation in a short period of time. Radiation therapy has been given in small doses of daily radiation over a period of 6 to 7 weeks, to give time for the irradiated normal tissue to repair itself between the treatments and to minimize the acute toxicity from RT. SART delivers a similar dose of RT in just 3 to 5 treatments. This is only possible because of the recent improvements in the technology used to deliver the SART. The planning process and the computerized mechanism to shape the RT fields have improved significantly, so a high dose of RT can be delivered to the tumor target volume with a sharp fall off the RT dose to the surrounding normal tissue. Equally important, our machine is able to obtain a 3-D CT scan of the tumor region of the patient just before each treatment, so the radiation can be delivered accurately as planned. With these advances, high dose RT is delivered with limiting the radiation to the normal surrounding organs. A presentation at the 2014 Chicago Multidisciplinary Symposium in Thoracic Oncology reported only about 13 % of grade 1-3 side effects, and no grade 4 or 5 toxicity over 10 years of SART at Cleveland Clinic. SART is a very good option to treat early stage non-small cell lung cancer when surgery is not a plausible option. There is no head-to-head control of high 80 % to low 90 % at 2 to 3 years, and low 70 % at 5 years, which comparable to the results of surgical resection. A prospective phase II clinical trial by The Radiation Therapy Oncology Group, in fact, reported 3 year control in the treated lung tumor 98 %, and control in the treated tumor and involved lung lobe of 91 % using SART in medically inoperable patients. Phase III randomized trials comparing SART with surgery in healthy patients who can undergo surgery have been attempted, but they were closed due to poor accrual. It was difficult to ask patients to allow a study to choose for them to either undergo SART involving 3 to 5 outpatient treatments with expected mild side-effects, versus surgical resection to undergo anesthesia and thoracotomy that result in hospitalization with expected chest wall pain and reduction in pulmonary function. At Houston Precision Cancer Center, we have the modern technology, expertise, and extensive experience to use SART to treat patients with early stage lung cancer, hepatocellular carcinoma, oligometastases to the lung, liver, and brain.
Delivers concise radiation doses that conform to the size, shape, and location of the intracranial tumors while closely sparing healthy tissue.
Radiation therapy technique that combines intensity modulated radiation therapy (IMRT) with rotational arc delivery that consists of 360-degree rotation of the linear accelerator while the beam is focused on the target, sparing normal tissue.
Radiotherapy Cutting Edge Technologies
Linear accelerator that provides accurate, full-dose ranges for intensity-modulated radiation therapy (IMRT) and image-guided radiation therapy (IGRT).
Linear accelerator which has sophisticated fast image-guidance to accurately and precisely treat target tumors with speed.
Generates a specific CT scan that determines the location, shape, and size of the tumor to be treated with 4D gating scans allowing visibility of tumor movement and surrounding organs during the breathing cycle.

RADIOTHERAPY EXPERTS
Radiotherapy uses localized radiation to combat cancer. Our radiotherapists are trained to guide you through treatment, explain how it works, and give you the follow-up support you need.
